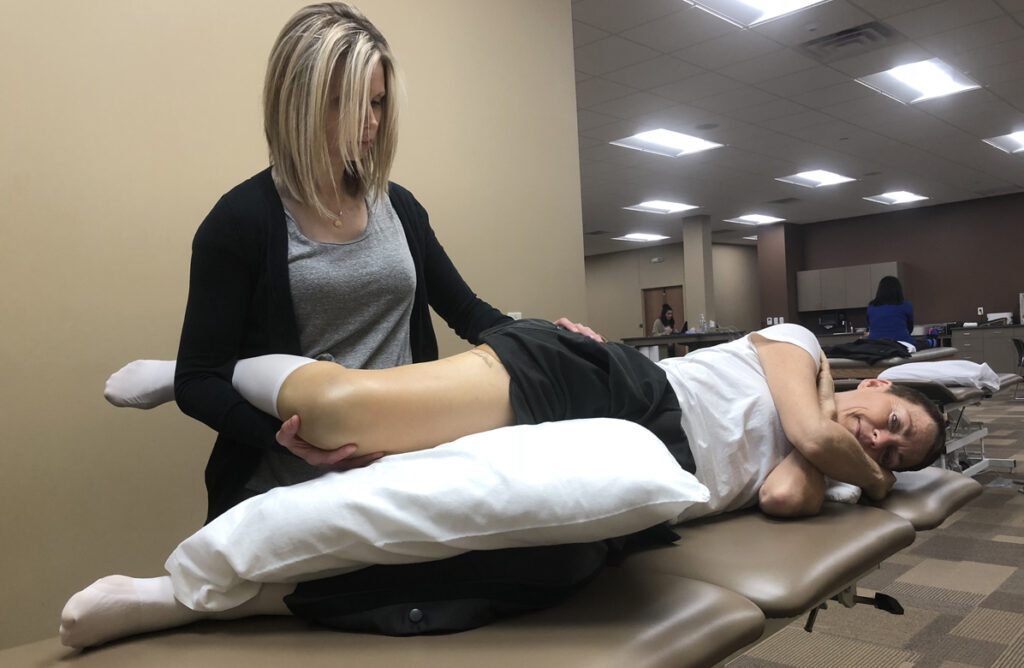
Part 5:
_____________________________________________________________
I Hate Feet and Other Tales of Post-Surgical Woe
By Susan Flansburg, ORA Orthopedics Hip Replacement Patient
In Part 5, Susan adjusts to post-surgery living and learns that putting on socks is not easy, and takes a willing helper!

The role of caregiver is key to your happiness as a patient. It may be too late for this advice, but choose carefully if you can.
For the first couple weeks following surgery, I needed help doing almost everything. My husband, Alan, would ensure I got into the shower safely (it is in a tub). He helped me out. He dried my feet.
On top of the expected discomfort and stiffness that impeded movement, I had to follow the dread “hip precautions” – what a mannerly word! – or risk a dislocation. The very thought terrified me. I couldn’t bend over or cross my legs. Would I ever be able to clip my toenails again? Or shave my legs?
Spoiler alert: Things do get better. But at the time, it seems like forever (especially, probably, for your caregiver).
Saint Alan began his service when he brought me home and got me situated after surgery. He was pretty enthusiastic then. As the days wore on, though, his good will ebbed a bit. Who can blame him? I’m not the ideal patient.
My cell phone was my service bell. Every time I needed something, I called him. He was one floor down, making dinner, feeding the dog, cleaning up from dinner. Can you get me some water? Can you adjust my covers? Can you rub my shoulders? You’re not doing it right!!!
I wasn’t surprised when, on the 3rd day, he grumbled I hate feet as he jabbed a towel at my wet toes after my shower. Nor was I shocked on Day #5 when he tossed a sock at me and said, “Put it on yourself!”
Meantime, I was feeling pretty sorry for myself. My right leg felt 6 inches longer than my left and twice as wide. When I sat down, it felt like I was sitting on one of Bear’s toys.
My right ankle looked like Great Aunt Hildegard’s.
And I couldn’t find anyplace to sit that was actually comfortable.
Physical Therapy
It’s amazing how fast they get you moving. The day of surgery, physical therapists get you walking. The day after, they teach you some exercises. On the third day (for me at least), they expect you to come to them for more exercises, and so on.
Beth lifted my leg into the car and drove me to my first post-surgery physical therapy appointment with Emily. Per her suggestion, I took a pain pill beforehand and was able to do the simple exercises she demonstrated.
It was a start, and gave me plenty to discuss with anyone who would listen. When I couldn’t find anyone, though, I resorted to my journal:
” … Emily says that my new hip may always feel different because it is not identical to my left hip. My body and brain will get used to it. And yes the swelling can cause some height discrepancy.”
“… Yesterday – 2 weeks after surgery – was the first day I felt energized almost until the end of the workday (I started back one week after surgery). I started to fade around 4 pm (after beginning my day at 4 am).”
“… Walked 4 blocks outside – first block arduous, rest got better.”
“… Slept much better just using Tylenol! Lots of swelling now in my ankle, though. This is my newest BIG problem. The problems just keep changing.”
“… Surprised by immense swelling. Need to elevate and do constant foot pumps. Another surprise: footwear does not fit as well when your foot is swollen.”
“… Had surgery follow-up with Dr. Martin’s physician assistant yesterday. Mark Hichborn assured me I’m doing great. He showed me the X-rays, and said that even though I feelone leg is longer than the other – many reasons for that, but very common – it’s not.”
“… My hip feels swollen and stiff this morning. And my main area of discomfort is my thigh, particularly the back of my thigh.”
“… Yesterday turned into a great day, with a mile walk along the Duck Creek bike path (Alan walking Bear), and book club at night! Of course, I had to stand up several times while the rest of the group continued to sit, and by 8 pm I was desperate to leave. Got home, in bed, and slept – with Tylenol – soundly.”
Tips:
- Swelling WILL happen. Elevate your leg when you can, do foot pumps (just move your feet up and down), and get up regularly.
- Go as easy as you can on your caregiver. Be sure to get what you need … but do you really NEED a glass of water given to you? It’s better for you to get up to fetch it yourself, anyway!
Up Next: “Sometimes it’s a Bumpy Road to Recovery” In Part 6 of Susan’s Journey, PT Emily’s prediction about surprises comes true. Hint: Cats are involved.
